Missing teeth can affect more than appearance: they change how you chew, speak, and even how your jawbone ages. Implant restorations address these issues by rebuilding both the foundation and the visible portion of the tooth. By anchoring replacement teeth to a biocompatible post embedded in the jaw, implant restorations restore function while preserving nearby healthy teeth. For patients seeking a durable, natural-feeling option, implants offer a predictable path back to a confident, fully functioning smile.
Unlike conventional bridges or removable prosthetics that rely on neighboring teeth or adhesives, implant restorations integrate with the bone to provide a stable support similar to a natural tooth root. That stability helps maintain jawbone volume and facial structure over time, reducing the gradual changes that can occur after tooth loss. For many patients, this combination of aesthetic and structural benefits makes implant restorations an appealing long-term investment in oral health and quality of life.
Choosing implant restorations is a collaborative process between patient and clinician. We evaluate each person’s oral health, habits, and restorative goals to recommend solutions that balance strength, appearance, and comfort. Clear communication and a personalized plan help patients set realistic expectations and feel confident about their treatment path from start to finish.
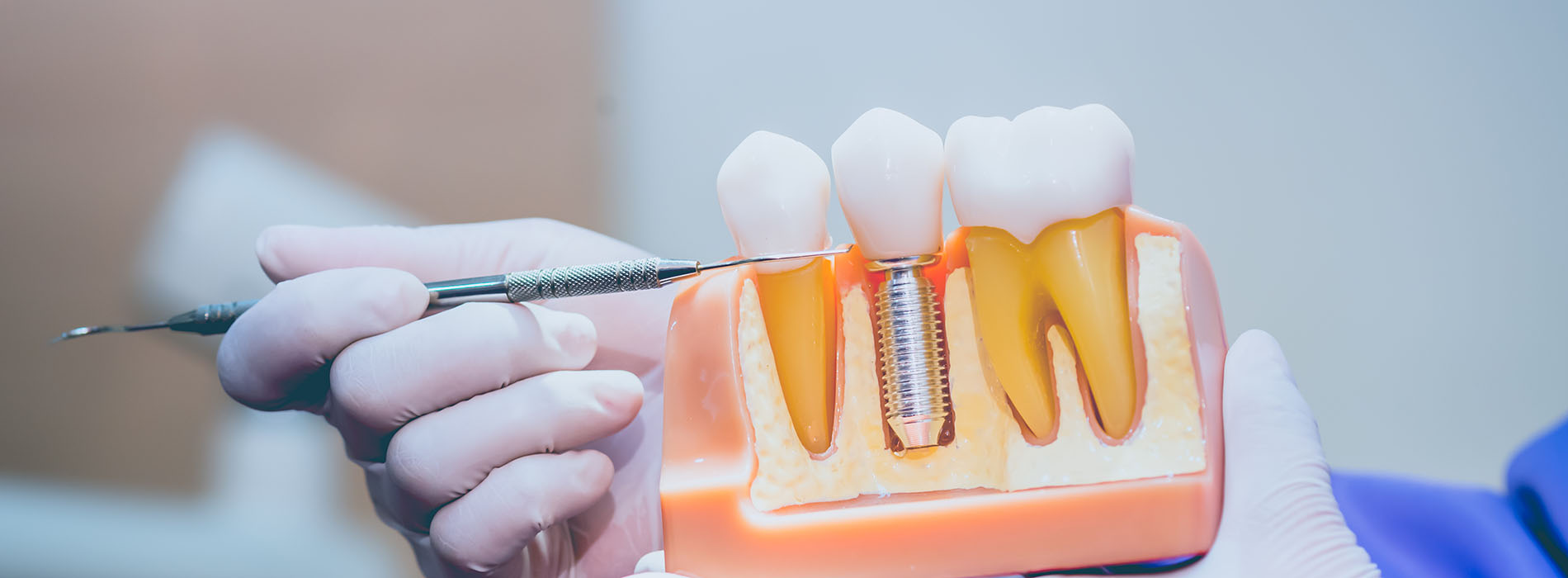
Dental implants are small, medical-grade posts—most commonly titanium—that serve as artificial tooth roots. After careful planning and placement into the jawbone, the implant undergoes osseointegration, a natural process where bone cells grow around the post and lock it into place. This biological fusion creates a strong, stable platform capable of supporting crowns, bridges, or implant-retained dentures with functionality similar to natural teeth.
When the implant has fully integrated, an abutment is attached to connect the post to the visible restoration. The final crown or bridge is then fabricated to match the color, shape, and bite of the surrounding dentition. Advances in materials and digital planning mean restorations can be highly customized—balancing strength with a lifelike appearance so the result looks and feels natural in everyday use.
Planning is an essential part of success. Digital imaging, careful evaluation of bone volume, and consideration of occlusion (how your teeth come together) allow clinicians to position implants precisely for long-term performance. Good case selection and adherence to clinical protocols minimize complications and help patients achieve predictable, satisfying outcomes.
The restorative journey begins with a comprehensive consultation where the dental team reviews your health history, takes diagnostic images, and discusses goals and expectations. If implants are appropriate, a treatment plan is developed outlining the number of implants needed, the type of restoration (single crown, bridge, or denture), and the general timeline. This planning phase ensures both patient and clinician understand the sequence of care and desired esthetic results.
Surgical placement of the implant is a minor outpatient procedure performed with appropriate anesthesia and comfort measures. Following placement, a healing period allows the implant to integrate with the bone. Once integration is confirmed, the restorative phase begins: impressions or digital scans are taken to craft the custom crown or bridge, and the final restoration is secured to the implant abutment. Patients can expect follow-up visits to assess healing and fit during this period.
Some cases qualify for immediate restoration protocols where a temporary tooth is placed at the same visit as the implant, but suitability depends on factors like bone quality and bite forces. Regardless of timing, the goal is the same: return you to normal function and a natural-looking smile while respecting biologic healing and long-term stability.
Designing an implant restoration involves both engineering and artistry. Materials such as porcelain-fused-to-zirconia or all-ceramic crowns are often chosen for their strength and translucency, mimicking the light-reflective qualities of natural enamel. For larger spans, bridges or hybrid prostheses can be engineered to withstand biting forces while maintaining a lifelike appearance. The lab work and shade-matching process are essential to ensure your restoration blends seamlessly with the adjacent teeth.
Beyond aesthetics, the connection between implant and restoration is engineered to distribute chewing forces effectively. Properly designed occlusion and precise fit reduce stress on the implant and surrounding bone, enhancing longevity. In some restorative designs, screw-retained restorations are used to facilitate maintenance and retrieval if future repairs or adjustments are needed without disturbing the implant itself.
Attention to detail—including the emergence profile, margin placement, and soft-tissue shaping—helps the restoration look natural at the gumline. Careful coordination between clinician and dental laboratory produces results that not only function well but also contribute positively to facial balance and overall confidence when smiling and speaking.
While implant restorations are resistant to decay, the surrounding soft tissues and supporting bone still require attention. Daily oral hygiene—brushing twice and cleaning between teeth with floss or interdental brushes—is essential to remove plaque and prevent inflammation around the implant. Regular professional cleanings allow the dental team to monitor tissue health, assess occlusion, and remove deposits in hard-to-reach areas.
Routine checkups play an important role in early detection of potential problems such as loosening components, wear on the restoration, or changes in bite. Periodic radiographs help evaluate bone levels around the implants and ensure the long-term stability of the restoration. If issues are identified early, many problems can be managed conservatively without complex intervention.
Healthy habits also contribute to the longevity of implant restorations. Avoiding tobacco, managing bruxism (tooth grinding) with protective appliances when recommended, and maintaining overall oral health support the life expectancy of implants. With consistent care and periodic professional oversight, implant restorations can serve patients reliably for many years.
Summary: Implant restorations offer a reliable, tooth-preserving solution for replacing missing teeth by combining the stability of an anchored implant with custom-made restorative work that looks and functions like natural dentition. The process blends clinical planning, skilled surgical placement, and precision restoration to rebuild comfort, chewing ability, and confidence. If you’d like to learn more about how implant restorations might fit your needs, please contact us for additional information and to arrange a consultation with our team at the office of Christopher R. Szydelko, DDS PC.
Implant restorations replace missing teeth by combining a biocompatible post implanted into the jaw with a custom-made visible restoration such as a crown, bridge or denture. The implanted post acts as an artificial root and provides a stable foundation for chewing and speaking that closely mimics natural tooth function. The restorative component is then attached to an abutment and shaped and shaded to blend with surrounding teeth.
Unlike conventional bridges or removable prosthetics that rely on adjacent teeth or adhesives, implant restorations integrate with bone to deliver long-term stability and preserve nearby tooth structure. Because they support the jawbone, implants help reduce the bone resorption and facial changes that can follow tooth loss. This combination of structural support and cosmetic customization makes implant restorations a durable and natural-feeling option for many patients.
Good candidates for implant restorations generally have adequate bone volume at the implant site, healthy gums free of untreated periodontal disease, and overall medical conditions that support healing. Routine medical issues such as controlled diabetes or a history of smoking require careful evaluation, but do not automatically exclude patients from receiving implants. A comprehensive examination including digital imaging helps determine whether bone grafting or other preparatory procedures are necessary to create a stable foundation.
Patient commitment to daily oral hygiene and regular dental visits is also essential because the long-term success of implants depends on maintaining healthy soft tissues and bone. Age alone is not a limiting factor; rather, the focus is on local anatomy and general health that influence surgical risk and healing. Your clinician will review your medical history, discuss goals, and recommend the best restorative pathway based on clinical findings.
The implant restoration timeline begins with a consultation and diagnostic imaging to plan implant position and evaluate bone quality, and then proceeds to surgical placement of the implant post. After surgery there is a healing period during which osseointegration occurs; this phase commonly ranges from a few months to several months depending on bone density, implant stability and whether grafting was performed. Once integration is confirmed, the restorative phase begins with impressions or digital scans to fabricate the custom abutment and final restoration.
Some cases qualify for immediate or early provisional restorations placed on the same day as implant placement, but suitability depends on factors such as primary stability and bite forces. Follow-up visits monitor healing, soft-tissue response and occlusion to ensure the final restoration fits and functions correctly. Because individual anatomy and treatment complexity vary, your clinician will provide a personalized timeline during the planning visit.
Implant restorations are commonly fabricated from materials such as all-ceramic (zirconia or lithium disilicate), porcelain-fused-to-zirconia, or porcelain-fused-to-metal, each offering a balance of aesthetics and durability. All-ceramic materials provide excellent translucency and lifelike appearance for front teeth, while high-strength ceramics and metal-ceramic combinations are often selected for posterior restorations where biting forces are greater. The laboratory process includes careful shade matching and contouring to achieve a natural emergence profile and seamless integration with adjacent teeth.
Restorations can be designed as screw-retained or cement-retained, and each option has practical implications for retrievability and maintenance. Screw-retained restorations facilitate easy removal for repairs or adjustments without disturbing the implant, while cement-retained crowns may provide certain esthetic or angulation advantages when carefully managed. Your clinician will recommend materials and retention methods based on functional needs, esthetic goals and long-term maintenance considerations.
Osseointegration is the biological process by which bone cells grow onto and around the surface of the implant post, creating a rigid, stable connection between bone and implant. This process typically takes several weeks to months and is essential because it allows the implant to function like a natural tooth root under chewing forces. Successful osseointegration protects against micro-movement of the implant and provides the foundation needed for long-term load-bearing restorations.
Because an integrated implant transmits chewing forces into the jawbone, it helps maintain bone volume and facial structure that otherwise can diminish after tooth loss. Proper surgical technique, implant design, and patient factors such as bone quality and oral hygiene all influence the likelihood and speed of osseointegration. Regular monitoring with clinical exams and radiographs ensures bone levels remain healthy over time.
Yes. Implant restorations are versatile and can replace a single missing tooth, span multiple missing teeth with implant-supported bridges, or anchor full-arch prostheses such as implant-retained dentures. Strategic placement of several implants can provide stable support for dentures that are more secure than traditional removable options, improving chewing efficiency and patient comfort. Techniques such as All-on-4® or All-on-6® use a limited number of implants to support a full-arch prosthesis and are designed to maximize bone support and restorative stability.
The design of a multi-unit restoration considers force distribution, hygiene access, and prosthesis retrievability to allow for routine maintenance. Treatment planning for larger restorations often involves 3D imaging and close coordination with the dental laboratory to ensure proper fit and esthetics. Your clinician will evaluate jaw anatomy and functional demands to recommend the most appropriate implant-supported solution for multiple missing teeth.
Implant placement is typically an outpatient procedure performed with local anesthesia and optional sedation to ensure patient comfort. During the surgery the clinician prepares the implant site, positions the implant post into the bone and may place a healing abutment or cover screw; the procedure duration varies with the number and complexity of implants. After surgery patients should expect mild swelling, minor discomfort and temporary dietary adjustments while tissues begin to heal.
Postoperative care includes following prescribed oral hygiene instructions, taking any recommended medications, and attending follow-up visits to monitor healing. Stitches are often removed or evaluated within one to two weeks, and radiographs may be taken to assess implant position and early integration. Most patients return to normal activities within a few days, but full integration and final restoration placement require the healing interval determined during planning.
Daily oral hygiene is essential for preserving implant health and includes brushing twice a day with a soft-bristled brush and cleaning between teeth and implants using floss, interdental brushes or water irrigation as recommended. Effective plaque control around the restoration and at the gumline helps prevent inflammation of the soft tissues that support the implant. Regular professional cleanings and periodic radiographs allow the dental team to monitor tissue health, detect early changes and remove deposits in hard-to-reach areas.
Patients with parafunctional habits such as bruxism should discuss protective options like night guards to reduce excessive forces on the restoration. Avoiding tobacco and managing systemic health conditions also supports healing and long-term implant stability. Consistent follow-up care and prompt attention to any changes in bite, mobility or tissue health help protect your investment and maintain function for years to come.
Complications can include soft-tissue inflammation (peri-implant mucositis), progressive bone loss around the implant (peri-implantitis), loosening of restorative components, or wear and fracture of the prosthetic material. Early signs such as redness, bleeding on probing, increased pocket depth or mobility require timely evaluation because early intervention often prevents more significant problems. Management strategies range from non-surgical cleaning and improved home care to surgical intervention and component replacement depending on severity.
Proper case selection, precise surgical technique and ongoing maintenance reduce the risk of complications, while occlusal adjustments and addressing parafunctional habits minimize mechanical overload. If a restorative component becomes loose or damaged, screw-retained designs often allow straightforward retrieval for repair without disturbing the implant. Your dental team will explain monitoring protocols and treat issues conservatively when possible to restore function and tissue health.
Immediate restoration is considered when implants achieve sufficient primary stability at placement, when bone quality supports immediate loading, and when occlusion and esthetic requirements are favorable. The clinician evaluates insertion torque, bone density, soft-tissue conditions and overall bite dynamics to determine whether a provisional restoration can be safely attached without jeopardizing osseointegration. Immediate protocols can provide esthetic and functional benefits but require careful case selection to avoid early failures.
Decisions about immediate restoration are made on a case-by-case basis after comprehensive imaging and planning, and they include contingency plans should primary stability be lower than anticipated. Your clinician at the office of Christopher R. Szydelko, DDS PC will review the risks and benefits, explain the expected timeline, and recommend the most predictable approach based on your anatomy and treatment goals.
