A dental filling does more than patch a hole — it restores a tooth’s strength, preserves its shape, and protects the surrounding tissues from further damage. When decay or trauma removes healthy enamel and dentin, a restorative material is used to rebuild the tooth so it can chew, speak, and look like it did before the problem began. Thoughtful restoration helps prevent future fractures and can extend the life of the natural tooth for many years.
Fillings are among the most common services provided in general dentistry because tooth decay remains widespread across all ages. The goal of contemporary restorative care is to remove disease while conserving as much healthy tooth structure as possible. That balance — preservation plus protection — is what separates routine repair from durable oral health management.
Patient comfort, evidence-based techniques, and aesthetic outcomes go hand in hand in our approach. A well-placed filling should be functionally reliable, blend naturally with the tooth, and be maintained easily with regular home care. These are the fundamentals we emphasize whenever a restoration is recommended.
Humans have sought ways to treat damaged teeth for millennia. Early attempts at sealing or replacing decayed areas appear in archaeological records from long ago, but modern restorative materials developed most rapidly over the last two centuries. Metal alloys, including gold and amalgam, dominated early restorative dentistry due to their strength and longevity.
Over recent decades, materials science and adhesive technology have reshaped how clinicians restore teeth. Tooth-colored composites, ceramics, and glass ionomers offer options that combine strength with a natural appearance. These advances allow clinicians to match restorations to the patient’s smile while using techniques that bond materials directly to remaining tooth structure.
Clinical decisions about fillings are guided by the extent of damage, location in the mouth, functional demands, and aesthetic goals. We begin with a careful evaluation, including clinical examination and any necessary imaging, then present options that protect long-term health while respecting the patient’s preferences. Our objective is to choose the treatment that best preserves the tooth and supports overall oral wellness.
When appropriate, conservative techniques that require less removal of sound tooth tissue are favored. Patients are walked through each step of care so they understand why a material or method is recommended. Clear communication and predictable outcomes are the cornerstones of our restorative philosophy at Christopher R. Szydelko, DDS PC.
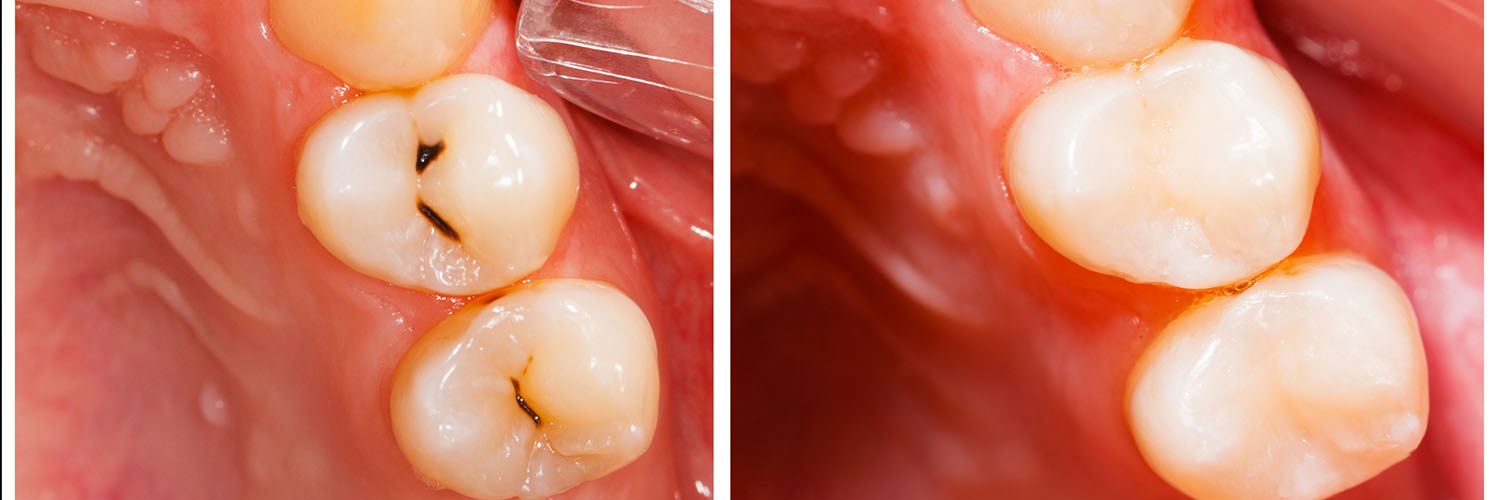
There is no single “best” filling material for every situation. The choice depends on factors such as the size and location of the cavity, the amount of biting force the tooth will need to endure, and how visible the tooth is when you smile. Advances in dental materials give clinicians multiple options to balance strength, longevity, and appearance.
Some materials are placed directly in the mouth in a single visit, while others are fabricated outside the mouth and bonded in a follow-up appointment. Your dentist will explain the advantages and limitations of each option so you can make an informed decision tailored to your needs.
Durability, wear resistance, and how a material interacts with temperature changes in the mouth are also important considerations. Long-term success relies not only on the material chosen but on precise technique, proper isolation during placement, and ongoing oral care after the restoration is complete.
Composite fillings are popular because they can be closely matched to your natural tooth shade and bonded to the tooth surface. The bonding process helps seal the restoration and can strengthen weakened tooth structure. Composites are versatile and can be used to restore small to moderate cavities, correct minor shape issues, and improve the overall appearance of teeth.
While highly aesthetic, composite materials can be more susceptible to wear and staining over time compared with some indirect restorations. With appropriate care and periodic assessment, however, composite restorations provide excellent results for many patients.
Amalgam has a long history of dependable performance, particularly for posterior teeth that receive heavy chewing forces. These restorations are known for their durability and resistance to wear. Although not tooth-colored, amalgam remains a functional option in certain clinical situations where longevity is the priority.
Glass ionomers bond chemically to tooth structure and release fluoride, which can help protect the tooth from future decay. They are often used in situations such as restorations near the gum line, pediatric dentistry, or as a temporary solution. Because they are less wear-resistant than other materials, they are selected when conservative protection and fluoride release are important.
Ceramics offer excellent aesthetics and resistance to staining and wear. Indirect restorations like ceramic inlays or onlays are fabricated in a laboratory or milled in-office and then bonded to the tooth. These options are especially suitable for larger defects where a direct filling might not provide the most durable long-term outcome.
Gold is less commonly used today but remains an excellent restorative material. It is biocompatible, durable, and gentle on opposing teeth. In select cases where exceptional longevity and response to chewing forces are necessary, gold restorations can be an appropriate choice.
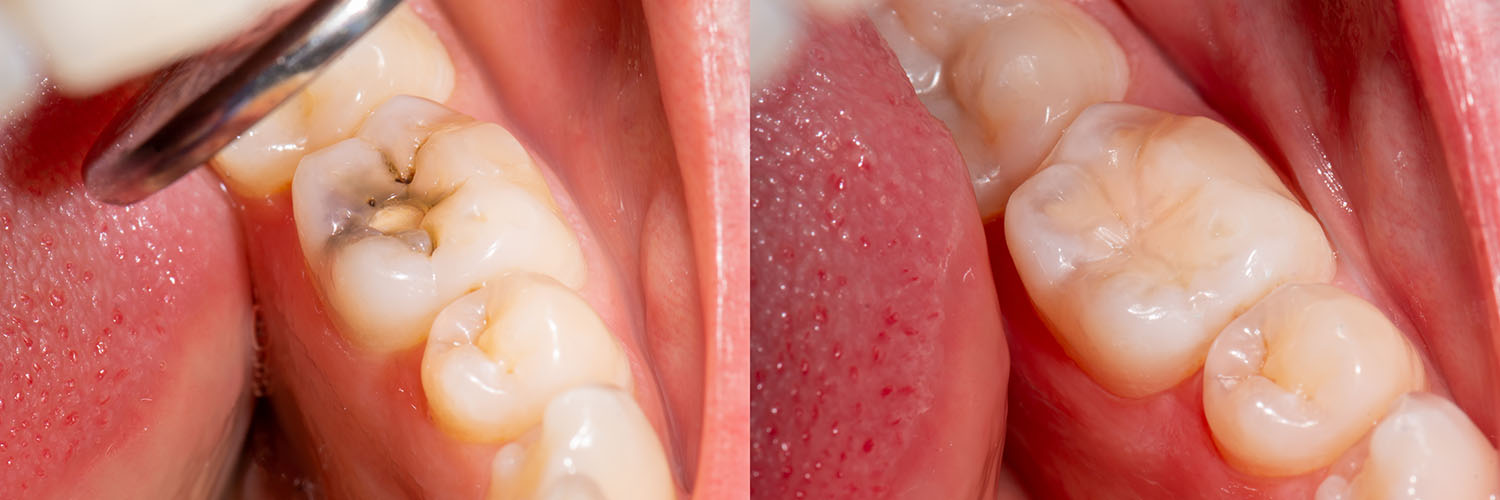
Not every damaged tooth is best treated with a simple filling. Larger cavities, cracks that extend into the tooth’s core, or restorations that have failed repeatedly may require more extensive care such as an inlay, onlay, crown, or root canal therapy. Recognizing when a conservative filling will suffice and when to escalate treatment is essential for protecting long-term tooth vitality.
Indirect restorations — those fabricated outside the mouth — often provide a stronger, more predictable outcome for significant defects. These options can preserve the remaining tooth while restoring function and appearance. Your clinician will discuss alternatives and the reasons one approach may be preferred over another.
Treatment planning considers both immediate needs and how the tooth is likely to perform over time. The goal is to select solutions that minimize future interventions while supporting optimal oral health and comfort.
A filling appointment typically begins with a focused exam and any necessary imaging to determine the extent of decay. Local anesthesia is commonly used to ensure the tooth and surrounding tissues are comfortable throughout the procedure. Once the area is numb, the decayed material is removed and the tooth is prepared to receive the chosen restorative material.
Depending on the material selected, the placement method will differ. Direct materials like composites are layered and cured in the mouth, while indirect restorations require impressions or digital scans and a subsequent appointment for cementation. Attention to isolation, bonding technique, and occlusal (bite) adjustments are critical steps that influence the long-term success of the restoration.
For patients who experience anxiety, many practices offer options to help you relax during care, including local anesthesia and procedural strategies for comfort. Your care team will explain the steps of the appointment and answer questions so you feel informed and at ease.
After a filling is placed, proper home care and routine dental visits are the best ways to protect your investment in oral health. Brushing twice daily with fluoride toothpaste, cleaning between teeth with floss or interdental brushes, and maintaining regular checkups help detect wear or small changes before they become larger problems.
It is normal for a restored tooth to feel slightly different at first. Minor sensitivity to temperature or pressure often resolves within days to weeks. If sensitivity increases, or if you notice persistent discomfort, contact the practice so the restoration can be evaluated and adjusted if necessary.
Regular professional assessments allow your clinician to monitor the integrity of fillings and recommend repair or replacement when appropriate. With attentive care, many modern restorations provide lasting function and a natural appearance for years.
Protect tissues while numb
Immediately after a procedure you may experience lingering numbness. Avoid chewing, sipping hot liquids, or touching lips and cheeks until sensation returns to reduce the risk of accidental injury.
Expect a period of adjustment
A restored tooth can feel different at first. Minor bite or surface sensations are common and often require only small polishing or adjustment if they persist.
Sensitivity is usually temporary
Short-term sensitivity to hot, cold, or pressure is not unusual after restoration. If sensitivity worsens or does not improve, schedule an evaluation.
Maintain your restoration
Good oral hygiene and routine dental care extend the life of fillings. Even the best restorations may need attention over time if decay recurs or the tooth sustains new damage.
If you have questions about fillings, restoration options, or which approach is best for your smile, please contact us for more information.
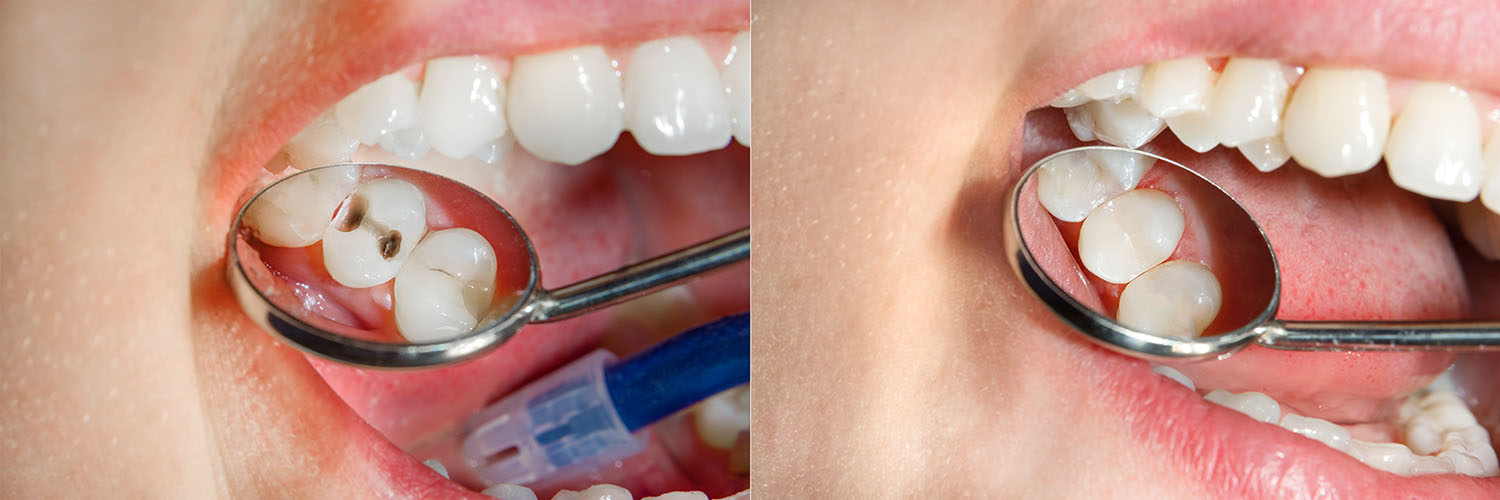
If the pleasure of eating a delicious bowl of ice cream or sipping a soothing cup of tea gets overshadowed by dental pain that makes you wince; it's time to contact our office. As skilled providers of care, we'll determine what's causing your discomfort and perform the treatment required to alleviate your symptoms and get you back on the road to oral health.
Cavities develop because of an infectious process that causes progressive damage to tooth structure. Despite starting as a pinpoint defect on the outermost enamel layer of your tooth, untreated dental decay progressively compromises more and more healthy tooth structure as it works its way to the inner layers of your tooth.
Yes, you can still develop tooth decay on other surfaces of the tooth, around the margins of an old filling, or in fewer instances, recurrent decay underneath it. For this reason, it's essential to maintain excellent oral hygiene, a diet low in sugary beverages and sweets, and be sure to visit our office for routine checkups and care. While tooth decay is second only to the common cold in frequency, it's almost entirely preventable.
We value the time and comfort of our patients. If cavities are located on adjacent teeth, or in the same section of your smile, it may be possible to treat more than one tooth during your visit. However, how much is done each visit depends on several factors. We keep our patients well informed and tailor every treatment plan and visit to address their unique needs.
Addressing concerns on the presence of elemental mercury in silver fillings, the American Dental Association (ADA), The Center for Disease Control and Prevention (CDC), the FDA, and the World Health Organization have all stated that amalgam restorations do not pose a risk to health. However, individuals with allergies or sensitivities to the metals in dental amalgam are advised to pursue other restorative options.
Dental fillings are performed under local anesthesia to help ensure your comfort throughout the entire procedure. The involved tooth remains completely numb for the extent of your visit. Within one or two hours after the procedure is completed, the local anesthetic will gradually wear off, and normal sensations return.
A tooth-colored composite filling is fully hardened and set by the end of your visit. However, we may advise you to wait a couple of hours until the local anesthesia has completely worn off. This advice is to help ensure you don't accidentally bite your lip, cheek, or tongue while still numb.
The lifetime of a dental filling varies depending on the type of material used. While popular dental materials can last a decade or more with proper care, they can degrade over time, wear down, or even break. When this happens, you may experience some tooth sensitivity, a jagged edge, or a loose or dislodged piece of filling material. Whatever the case may be, it's essential to get the filling replaced before the tooth sustains further damage or other consequences arise. Beyond taking good care of your smile to help ensure the longevity of your fillings, our office regularly checks the status of your existing fillings as part of a routine checkup exam.
Dental fillings are an essential investment that serves to preserve and protect the health of your smile. With that said, how much a filling costs depends on the number of surfaces of the tooth involved and the filling material that is used. Amalgam restorations are the most economical. While tooth-colored composite fillings have a slightly higher cost, they offer the added benefits of being metal-free and much more aesthetically pleasing. Ceramic fillings, inlays, and onlays are more expensive than the preceding options but provide outstanding, long-lasting, and natural-looking results.
Dental insurances typically cover the cost of dental fillings. While we work with you to maximize your insurance benefits, there may still be an out-of-pocket expense. At the office of Christopher R. Szydelko, DDS PC, we strive to help you begin care without any additional financial stress or delay.
Dental fillings are restorative materials placed in teeth to repair damage from decay or trauma and to restore normal form and function. A filling replaces lost enamel and dentin so the tooth can chew, speak, and maintain its shape while protecting surrounding tissues from further breakdown. By sealing the cavity and rebuilding structural integrity, a well-placed filling helps prevent fractures and reduces the risk of infection that could threaten the tooth’s long-term health.
Modern restorative care emphasizes conserving healthy tooth structure while removing diseased tissue, and that balance is central to achieving durable outcomes. Fillings are a cornerstone of preventive and restorative dentistry because they address active disease and limit the need for more invasive treatments later. Regular evaluation and proper oral hygiene help fillings perform as intended and support overall mouth health.
Choosing a filling material depends on the size and location of the defect, the amount of biting force the tooth will need to withstand, aesthetic concerns, and the condition of the remaining tooth structure. Clinicians evaluate clinical findings and any necessary imaging, then discuss options that balance strength, longevity, and appearance so the patient can make an informed decision. Some materials are placed directly in a single visit while others are fabricated outside the mouth and bonded in a follow-up appointment, and each approach has specific advantages depending on the situation.
Long-term success relies on both the material choice and the placement technique, including isolation, bonding protocol, and occlusal adjustment. For teeth that require substantial rebuilding or are subject to heavy chewing loads, indirect restorations such as inlays, onlays, or crowns may be recommended instead of a direct filling. The goal of the treatment plan is to preserve tooth vitality, minimize future interventions, and deliver predictable function and appearance.
Common materials include tooth-colored composite resins, traditional amalgam, glass ionomer cements, ceramic inlays/onlays, and gold restorations. Composite resins are popular for their aesthetic match to natural teeth and bonding properties, while amalgam has a long track record for durability in posterior teeth that endure heavy chewing forces. Glass ionomers bond chemically to tooth structure and release fluoride, which can be helpful in specific situations, and ceramics or gold are used when exceptional wear resistance and longevity are priorities.
Each material has trade-offs related to strength, wear resistance, esthetics, and suitability for particular clinical scenarios, so the decision is individualized. Advances in adhesive dentistry and materials science have broadened options and improved outcomes, allowing clinicians to tailor restorations to both functional demands and cosmetic goals. Your dentist will explain the reasons a particular material is recommended for your tooth based on these considerations.
A typical filling appointment begins with a focused exam and any necessary imaging to determine the extent of decay, followed by local anesthesia to ensure comfort. The decayed or damaged tooth structure is carefully removed, the preparation is shaped to receive the restorative material, and the area is isolated to keep it dry for bonding or placement. Direct materials such as composites are placed in layers and cured with a light, while indirect restorations require impressions or digital scans and a second visit for bonding the finished piece.
During placement the clinician pays close attention to bonding technique, margin integrity, and occlusion so the restoration functions properly within the bite. Final polishing and bite checks are performed to reduce roughness and prevent high spots that can cause discomfort or premature wear. Postoperative instructions will explain temporary sensitivities and steps to protect the restoration while tissues recover.
Most patients experience minimal discomfort during a filling because local anesthesia is used to numb the tooth and surrounding tissues before the procedure begins. With effective anesthesia and modern techniques, the actual preparation and placement should be pain free, and the dentist will monitor your comfort throughout the appointment. For patients who feel anxious or have special needs, behavioral strategies and additional comfort measures can be discussed in advance to make the visit as relaxed as possible.
It is common to have mild sensitivity or a different sensation in the restored tooth for days or weeks after treatment as the tooth adapts. This sensitivity typically diminishes on its own, but if numbness, increasing pain, or prolonged sensitivity occurs, contact the office for an evaluation. Prompt attention can identify whether an adjustment, further treatment, or protective measures are needed to maintain comfort and tooth health.
The lifespan of a filling varies depending on the material used, the size and location of the restoration, the quality of the placement, and the patient’s oral habits. Composite resins may wear or stain over time and can last many years with proper care, while amalgam and gold are known for long-lasting durability in certain situations. Eating habits, bruxism (tooth grinding), oral hygiene, and regular dental checkups all influence how well a restoration performs over the long term.
Routine professional exams allow your dentist to monitor restorations for wear, marginal breakdown, or recurrent decay and recommend repair or replacement when appropriate. Early detection of small changes can often be managed conservatively to preserve more tooth structure. Maintaining good home care and addressing habits like bruxism with protective devices can extend the functional life of fillings.
A filling may not be appropriate when decay or damage is extensive, when a crack extends into the tooth’s core, or when previous restorations have failed repeatedly and compromised the remaining tooth structure. In such cases, indirect restorations like inlays, onlays, or crowns are often a better choice because they provide greater strength and coverage for large defects. If the pulp is affected or infection has reached the nerve, root canal therapy followed by a protective restoration may be necessary to preserve the tooth.
Treatment planning looks beyond the immediate repair to how the tooth is likely to perform over time, and the clinician will explain alternatives and the rationale for recommending a more robust solution. The objective is to choose an approach that minimizes future interventions while maintaining comfort, function, and tooth vitality. Patients are encouraged to ask questions so they understand the benefits and limitations of each option.
After a filling is placed, patients should avoid chewing hard or very sticky foods on the treated tooth until any numbness has worn off and the restoration has settled. Maintain gentle but thorough brushing twice daily with fluoride toothpaste and clean between teeth with floss or interdental brushes to reduce the risk of recurrent decay. It is normal to experience mild sensitivity to temperature or pressure at first; this usually improves over days to weeks.
If you notice persistent discomfort, a change in bite, or roughness on the filling surface, contact the office so the restoration can be evaluated and adjusted if necessary. Regular dental checkups allow the clinician to monitor the integrity of restorations and catch small issues before they become larger problems. Following these simple care steps helps protect your restoration and supports lasting oral health.
Warning signs that a filling may need attention include persistent or worsening sensitivity, sharp pain when biting, visible cracks or gaps at the margin of the restoration, or dark discoloration around the filling. Recurrent decay can develop at the edges of an older filling and may be detected clinically or on radiographs during routine exams. A loose or missing filling is an urgent condition that should be addressed promptly to prevent further breakdown or infection.
Regular professional evaluations allow early detection of wear, marginal breakdown, or secondary decay so repairs can be made before the tooth becomes more compromised. Your dentist will recommend the least invasive and most predictable solution based on the extent of any problem, and in many cases timely repair preserves more natural tooth structure. If you experience any troubling symptoms between appointments, schedule an assessment to protect the restored tooth.
The practice follows evidence-based protocols that prioritize infection control, precise isolation, and proven bonding techniques to ensure predictable results. Careful clinical examination, appropriate imaging, and clear communication about material choices and procedural steps help patients understand their treatment and expected outcomes. Attention to occlusion, finishing, and polishing protects the restoration and reduces the risk of premature wear or postoperative issues.
At Christopher R. Szydelko, DDS PC the team emphasizes patient comfort, conservative tooth preservation, and ongoing monitoring to maintain long-term oral health. Regular follow-up visits allow clinicians to evaluate restorations over time and recommend maintenance or replacement when indicated. This systematic approach supports durable, functional, and natural-looking restorations for patients in and around Batavia.
